Thyroid issues are very common. Thyroid problems are usually discovered by a Primary Care doctor or maybe an OB/GYN during a routine physical examination or on a routine laboratory evaluation. Usually, patients are referred to an Endocrinologist for further evaluation. At the endocrinologist’s office, routine laboratory evaluations are performed in addition to an ultrasound of the neck. Patients who have nodules often require a biopsy. This is often referred to as a Fine Needle Aspiration. Biopsies are usually done on lesions that are approximately the size of a dime (1 cm) or bigger in size. If lesions are smaller than that, but have suspicious features for malignancy, they are also biopsied.
Depending on the biopsy results, you may or may not be referred for surgery. At your surgical evaluation, we will discuss not only your thyroid biopsy results, but we will also do another ultrasound on you. The result of ultrasounds can vary from office to office and they are very operator-dependant as far as who is performing them.
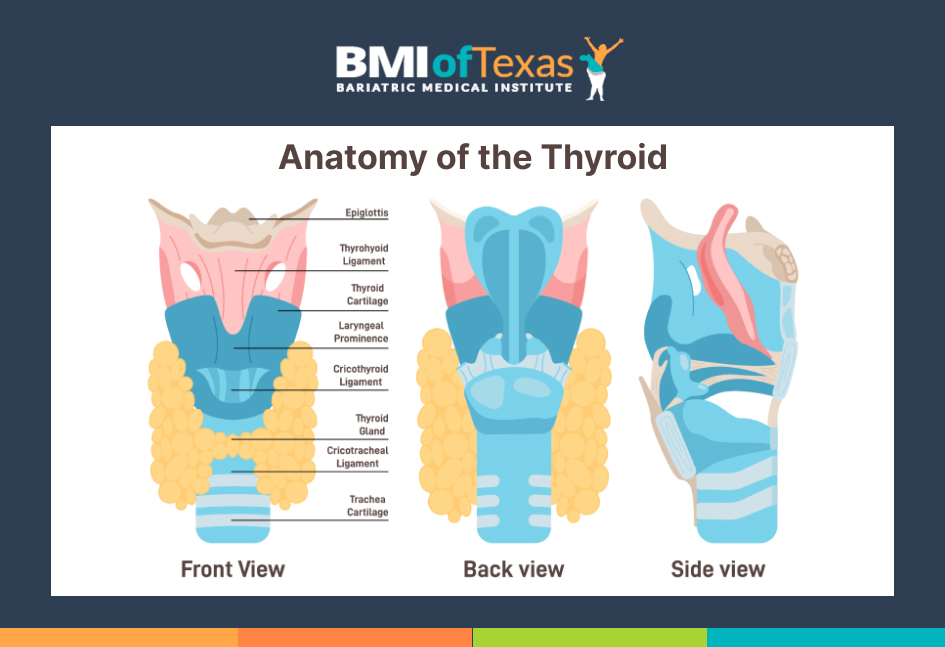
Thyroid biopsies
Results of biopsies come in several different ‘flavors.’ Benign lesions usually require follow-up on a routine basis with yearly biopsies done by your endocrinologist. If a Fine Needle Aspiration result is malignant, we usually recommend a complete removal of the thyroid. This is called a Total Thyroidectomy. Occasionally, biopsy results come back as ‘suspicious.’ When a lesion is suspicious, it is not for certain whether or not this is malignancy and usually further workup is recommended. This comes in the form of having a repeat Fine Needle Aspiration done by your endocrinologist and/or it could mean surgical excision of part of the thyroid gland to obtain the ‘ultimate biopsy.’ In these instances, the pathologist ultimately becomes the one who determines whether or not further treatment would then be required.
In addition, biopsy results can also be considered ‘insufficient.’ An insufficient biopsy means that there were not enough cells obtained in the needle when the biopsy was performed. In other words, you have a biopsy done on your neck and when the needle is inserted into the thyroid nodule, not enough cells from the thyroid nodule were captured inside the needle to be analyzed by the pathologist. In these cases, it is recommended that the patient undergo a repeat Fine Needle Aspiration or perhaps even surgical excision of that affected area to fully diagnose it.
A separate type of biopsy is called a ‘Follicular Lesion.’ Follicular lesions are usually benign. Doctors are unable to determine if follicular lesions are benign or malignant based on a Fine Needle Aspiration. In these instances, surgical excision is almost always recommended. Usually, we only have to remove only one-half of the thyroid gland. For example, if the lesion is on the left side of the neck, we would do a left thyroid lobectomy, or a removal of just the left lobe of the thyroid. At that time, the pathologist would then evaluate your thyroid specimen and determine whether or not the follicular lesion is benign or malignant.
In most cases, follicular lesions are benign. If the lesion is malignant, then we usually return to the operating room within the next several days to remove the other side. This would be called a completion thyroidectomy or complete removal of the remainder of the thyroid.
Surgery
Surgery usually takes about 1 – 1 ½ hours. This surgery is generally very safe. There are three main risks with surgery: injury to the recurrent laryngeal nerve, bleeding and hypocalcemia. The risk of injuring the recurrent laryngeal nerve is less than 1%; the risk of developing permanent hypocalcemia is also 1% or less, and the risk of bleeding is less than 1%. We make every effort in the operating room to identify all parathyroid glands and to preserve them at all cost at the time of surgery.
Recovery
After your thryroid surgery, you can anticipate one night in the hospital although some patients are able to go home the same day. After surgery, patients go to a regular hospital room, on a regular hospital floor, where they will be eating, drinking and walking on the night of surgery. In almost all cases, patients go home the following day.
When you go home from the hospital, there are very few restrictions on you. We ask that you do not drive a car for several days because your neck might be sore, and it may be difficult for you to turn side-to-side if you are driving. Otherwise, there are no major physical restrictions.
On occasion after a thyroidectomy, patients can develop symptoms of numbness and tingling around the fingers, tip of the nose and toes. This usually means that there is a hypocalcemia. Hypocalcemia means low calcium. The reason for this is that there are 4 very small parathyroid glands that live behind the thyroid. These parathyroid glands are responsible for calcium metabolism. During the course of thyroid surgery, these small glands can be injured, traumatized or temporarily ‘stunned’ and can cause you to have low calcium levels. This is usually self-limiting and goes away very quickly over the next couple of days or weeks.
After your discharge from the hospital, we usually see you in the office 2 to 3 weeks after surgery. In the meantime, we help you obtain an appointment with your endocrinologist where you will see him/her approximately 2 weeks after surgery. During that time, your endocrinologist will recheck your labs and make sure that your calcium and thyroid hormone levels are within normal limits.
Discharge from Hospital
When you are discharged from the hospital, you may be given synthetic thyroid medication, or Synthroid. The reason for this is that if we remove your entire thyroid, you will not be able to make any thyroid hormone. For this reason, we will have to give you synthetic thyroid and you can expect to be on this medication for the rest of your life. There are no major long-term side effects with long-term thyroid hormone replacement. Thyroid hormone replacement is usually quite inexpensive. Thyroid medications are controlled and managed by your endocrinologist or primary care provider.

